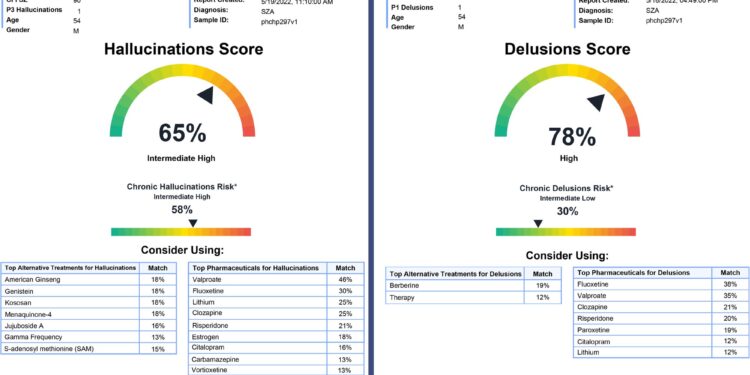
Example of a prototype report intended for doctors. Credit: Molecular Psychiatry (2024). DOI: 10.1038/s41380-024-02433-8
A team of researchers led by the Indiana University School of Medicine has developed a revolutionary new blood test for schizophrenia, a psychiatric disorder that includes hallucinations and delusions.
Schizophrenia and related psychotic disorders affect more than 3 million people in the United States. The new test identifies biomarkers in a person’s blood that can objectively measure their current severity and future risk of schizophrenia and match them to the most effective treatments for their individual biology.
“Schizophrenia is difficult to diagnose, especially at an early stage, and it is very important to match patients with appropriate treatment early on,” said Alexander Niculescu, MD, Ph.D., professor of psychiatry and neuroscience. medical studies at the IU School of Medicine. psychiatrist and researcher at the Richard L. Roudebush Veterans Administration Medical Center in Indianapolis and lead author of the study.
“Psychosis generally manifests itself in young adults, a privileged period of life. Stress and drugs, including marijuana, are triggering factors against a background of genetic vulnerability. If left unchecked, psychosis leads to accumulation of biological, social and psychological damage.”
In a study published in Molecular Psychiatry, researchers tested psychiatric patients whom they followed for more than a decade. They identified biomarkers predictive of strong hallucinations and elevated delusional states, as well as future psychiatric hospitalizations related to hallucinations and delusions. They also studied which biomarkers are the targets of existing drugs, which helps match patients to appropriate treatments.
Discovery, prioritization and validation of biomarkers for hallucinations and delusions. A, F Cohorts used in the study, describing the discovery flow, prioritization and validation of biomarkers at each stage. B, g Within-subject longitudinal analysis of the discovery cohort. Phchp### is the study ID for each subject. V# designates the visit number. VS, H Prioritization using convergent functional genomics (CFG). D, I Validation – biomarkers are assessed for incremental change from discovery subjects with no symptoms, with elevated symptoms to validation subjects with clinically severe symptoms, using ANOVA. The histograms represent an increased upper biomarker and a decreased upper biomarker (E, J.). Number of probe sets and scoring at each stage. Step 1: Discovery probe sets are identified based on their symptom tracking score and ranked at 33% (2 pts), 50% (4 pts), and 80% (6 pts). Step 2 – Prioritization with CFG for prior evidence of involvement in psychotic disorders. Maximum of 12 pts. Genes obtaining at least 6 pts out of a possible maximum of 18 pts after discovery and prioritization are reported to the validation stage. Step 3- Validation in an independent cohort of psychiatric patients with clinically severe hallucinations (P3 or P1 ≥ 4, PANSS ≥ 21) We selected the best CFE score ≥ 14 (not = 98 for hallucinations, not = 70 for delusions) for further testing and characterization. Credit: Molecular Psychiatry(2024). DOI: 10.1038/s41380-024-02433-8
The work builds on previous research conducted over the past two decades by Niculescu and colleagues on blood biomarkers of other psychiatric disorders (mood disorders, anxiety, post-traumatic stress disorder, suicide risk, pain and memory problems).
Niculescu said that in general, the best biomarkers were more predictive than standard scales used to assess someone suffering from hallucinations or delusions, meaning that using this biomarker test can help reduce subjectivity and the uncertainty of psychiatric evaluations.
“Fortunately, biologically, some of the existing drugs work very well if started early in the right patients,” Niculescu said. “Social support is also paramount, and once that and medications are in place, psychological support and therapy can also help. There is still much to understand and apply about cognition and its abnormalities, but there is reasons for optimism in this era of emerging precision psychiatry.
More information:
MD Hill et al, Precision medicine for psychotic disorders: objective assessment, risk prediction and pharmacogenomics, Molecular Psychiatry(2024). DOI: 10.1038/s41380-024-02433-8
Provided by Indiana University School of Medicine
Quote: A research team develops a blood test to predict the risk of psychosis and the most effective treatments (February 8, 2024) retrieved February 8, 2024 from
This document is subject to copyright. Apart from fair use for private study or research purposes, no part may be reproduced without written permission. The content is provided for information only.