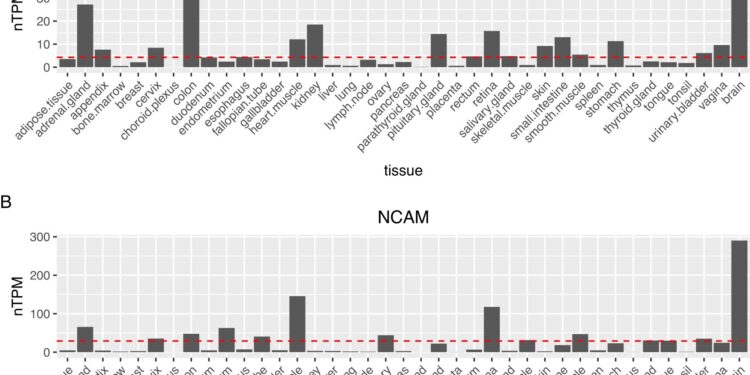
Proteins used for the isolation of EVs of neuronal origin lack brain specificity. The expression of L1CAM and NCAM mRNA in different tissues based on the Human Protein Atlas is plotted as normalized TPM values. The dotted red line represents 10% of brain expression, which corresponds to the threshold we set to exclude genes that exceeded this expression level in tissues other than the tissue of interest. This was the threshold used to identify placenta-specific EV mRNAs. Credit: Molecular Psychiatry (2024). DOI: 10.1038/s41380-023-02384-6
Researchers in a Johns Hopkins Children’s Center study that used genetic material from human blood and lab-grown brain cells say they have made progress in developing a blood test to identify brain changes associated with disease specifically linked to postpartum depression and other psychiatric disorders. and neurological disorders.
The research results, published January 11 in Molecular Psychiatry, focused on identifying the “fingerprints” of brain cell-derived mRNAs in the blood circulating outside the brain. These blood extracellular vesicles carry specific pieces of genetic material to the brain that potentially allow researchers to detect disease-associated changes in gene activity inside the brain.
Extracellular vesicles (EVs), fat bags of genetic material essential for communication between cells, carry messenger RNA (mRNA) and are released by all tissues in the body, including the brain.
The new research was inspired, investigators say, by the results of a study published in September 2022, in which Johns Hopkins Medicine scientists found that EV communication is impaired in pregnant women who develop postpartum depression after childbirth.
“We only detected placenta-specific EVs during pregnancy and not after birth. This was a proof of concept that we can detect EVs originating from a tissue or organ specific,” says Sarven Sabunciyan, Ph.D., assistant professor. of Pediatrics at Johns Hopkins University School of Medicine and senior author of the article.
First, using the human placenta as a model, investigators identified 26 placental mRNAs present in maternal blood only during pregnancy and not after birth, proving that mRNAs from specific tissues are found in circulating blood EVs.
Then, using lab-grown human brain tissue derived from stem cells (brain organoids), researchers found that EV mRNAs released from these brain tissues reflected changes occurring inside the tissues. Sabunciyan and his team conclude that it is possible to gather biological information about normally inaccessible tissues, such as the placenta and the brain, by examining EV mRNAs circulating in the blood.
They were able to identify mRNAs specifically expressed in the brain using data from the Human Protein Atlas (a Swedish database of human proteins found in cells, tissues and organs) and Genotype-Tissue Expression Project, which has extensively cataloged mRNAs. levels in human tissues.
Further analysis of these mRNA gene pathways showed that brain-specific mRNAs in blood EVs were involved in particular brain functions and were significantly enriched in genes already associated with brain disorders involving mood, schizophrenia , epilepsy and drug addiction.
The research team says this analysis suggests that these mRNAs are likely ideal biological markers for identifying such conditions.
“This is very exciting because currently there are no blood markers for disorders affecting the brain,” says Lena Smirnova, Ph.D., assistant professor in the Department of Environmental Health and Engineering at the Johns Hopkins Bloomberg School of Public. “Health and co-author of the article. Essentially, these conditions are diagnosed through clinical interviews between patients and providers.”
The researchers also discovered 13 brain-specific mRNAs in the blood that were associated with postpartum depression. To determine how well blood EV mRNAs reflect transcription in the brain, the researchers compared mRNAs isolated from cells and EVs in a brain organoid model. They found that although cellular and extracellular mRNA levels are not identical, they correlate and it is possible to extrapolate changes in cellular expression in the brain via EV mRNA levels.
The goal is to develop a simple blood test to detect changes such as higher or lower levels of EV mRNA in the blood directly linked to brain changes associated with mental disorders without having access to the brain itself, Sabunciyan says.
Ultimately, Sabunciyan adds, the availability of such blood tests could help detect early signs of mental health emergencies, such as suicidal behavior. The ability to identify patients at risk of suffering a psychiatric episode would allow the healthcare team to intervene and possibly prevent negative consequences.
In future studies, they plan to use lab-grown brain samples to identify similar biomarkers to develop tests for autism spectrum disorders.
The researchers caution that the differences identified in depression could be related only to postpartum depression, as the study was conducted using samples from only female participants.
More information:
Lena Smirnova et al, Blood extracellular vesicles carrying brain-specific mRNAs are potential biomarkers for detecting gene expression changes in the female brain, Molecular Psychiatry (2024). DOI: 10.1038/s41380-023-02384-6
Provided by Johns Hopkins University
Quote: Progress toward developing blood tests for psychiatric and neurological disorders (February 7, 2024) retrieved February 7, 2024 from
This document is subject to copyright. Apart from fair use for private study or research purposes, no part may be reproduced without written permission. The content is provided for information only.